The prospect of monitoring blood sugar continuously, painlessly, and without inserting anything into the body has driven research for more than four decades. For the more than 500 million people worldwide living with diabetes, and the hundreds of millions more with prediabetes or metabolic health concerns, a truly non-invasive continuous glucose monitor would represent one of the most meaningful quality-of-life advances in medical technology. In 2026, the technology is closer than it has ever been — but a fully approved, clinically validated, consumer-ready non-invasive glucose monitor that rivals the accuracy of existing systems still does not exist. Understanding why requires understanding both the genuine progress that has been made and the specific technical barriers that have defeated over 200 research programs since the 1980s.
The Current Standard: Minimally Invasive CGM
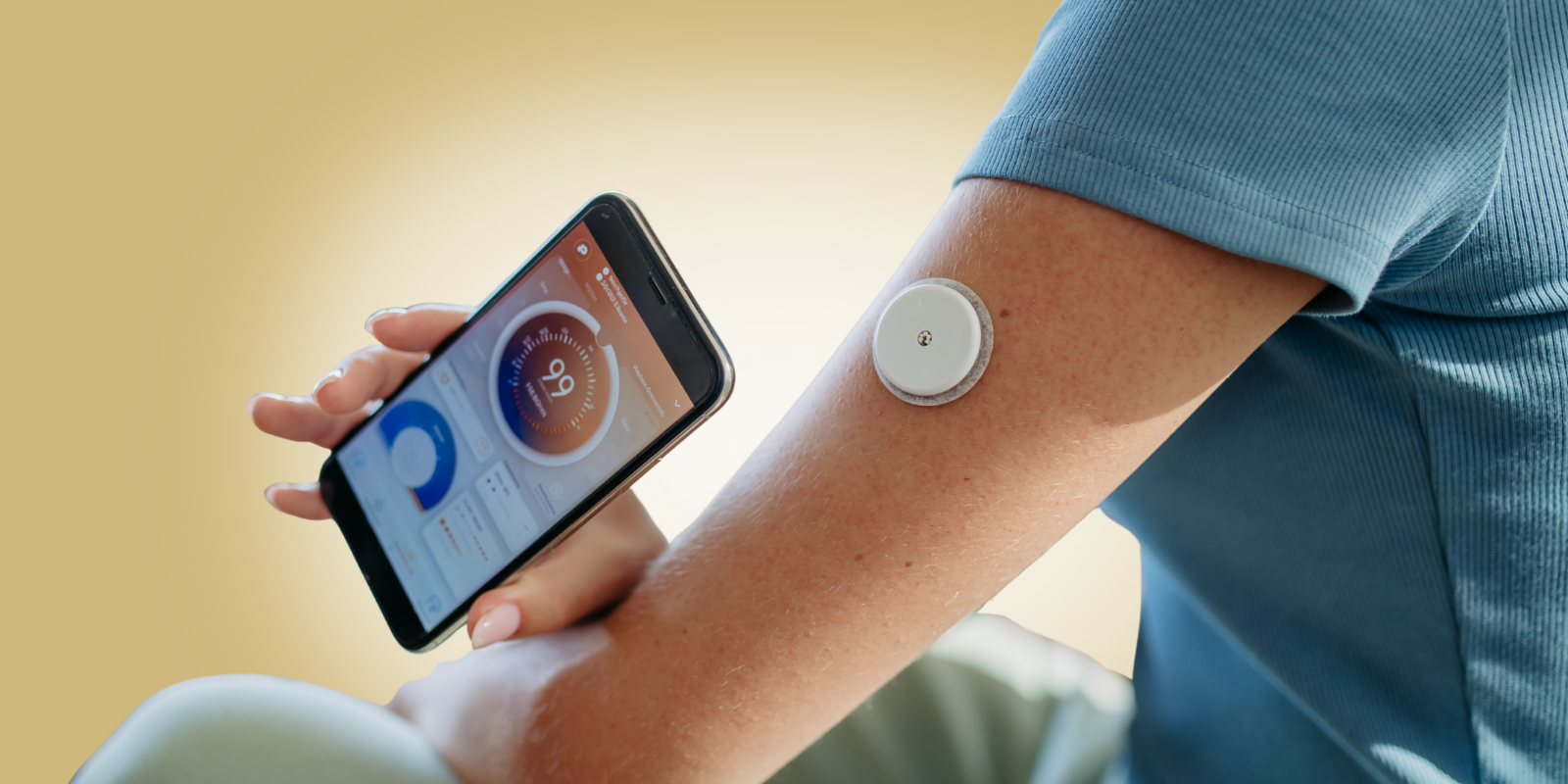
Before examining the needle-free frontier, it is worth establishing how advanced current continuous glucose monitoring already is. Dexcom’s Stelo, launched in 2024 as the first over-the-counter continuous glucose biosensor available without a prescription in the United States, uses a small sensor filament inserted just beneath the skin to measure glucose in interstitial fluid continuously. Abbott’s FreeStyle Libre system operates on the same principle and is available across dozens of countries. These devices are not truly non-invasive — they require inserting a small wire under the skin — but they have eliminated the need for multiple daily finger pricks and have transformed diabetes management for millions of patients.
The next generation of minimally invasive CGM is already in development. Abbott is developing a dual glucose-ketone sensor that can measure both metrics simultaneously in real time, offering early warning of diabetic ketoacidosis — a dangerous complication. Dexcom is reportedly working on a similar multi-analyte sensor. The Eversense system, which uses an implantable CGM that sits several centimeters beneath the skin and connects to a pump, was preparing for a limited launch in early 2026 marking the first connection between an Eversense device and an insulin pump.
The Non-Invasive Challenge: Why It Is So Difficult
The fundamental challenge is measurement specificity and signal noise. Glucose molecules in interstitial fluid are present in tiny concentrations relative to the surrounding biological material. Any optical, electromagnetic, or acoustic technique that attempts to detect glucose through the skin must overcome the interference of water, fat, protein, hemoglobin, and dozens of other biological compounds that absorb or scatter the measuring signal in ways that vary between individuals, between different body locations, and over time with changes in temperature, hydration, and activity level.
More than 200 different groups have pursued non-invasive glucose monitoring since the 1980s. Apple, Samsung, and Google have all initiated research programs in this area, and none have brought a product to market. The FDA’s accuracy threshold of ±15 mg/dL is demanding, and few devices consistently pass human trials.
What Is Actually Available in 2026
The most significant regulatory milestone as of 2026 belongs to Biolinq’s Shine patch — which received FDA clearance as a glucose-range sensor for the forearm for adults over 22 years with type 2 diabetes not using insulin. Notably, it is a glucose-range sensor, not a full CGM: it indicates whether glucose is in range or out of range rather than providing numeric values or trend arrows. This is a clinically meaningful distinction. A device that can tell you whether you are broadly in or out of range offers awareness value, but it cannot replace a full CGM for dosing decisions or for patients requiring precise glucose tracking.
Afon Technology, a Welsh startup developing the Glucowear device using radiofrequency technology worn beneath a smartwatch, reported entering clinical trials in 2025 ahead of an anticipated launch in 2026. The company has not yet received regulatory approval, and the clinical trial data has not been independently published at the time of this writing.
MIT researchers have developed a non-invasive glucose monitoring system based on Raman spectroscopy — a technique that analyzes how near-infrared light scatters when it encounters different molecules in tissue. Tests in volunteers showed accuracy comparable to commercially available under-skin CGM sensors. The device is currently being tested in a small clinical study at the MIT CCTR, with a larger study involving people with diabetes planned. The researchers are working toward a prototype the size of a watch.
The Consumer Electronics Giants and Their Timelines
Apple and Samsung have both confirmed ongoing research into non-invasive glucose monitoring, and both have published related patents. Samsung announced plans to incorporate glucose monitoring into its smartwatch in 2022, targeting 2025, but as of early 2026 has not confirmed whether or how this feature has been implemented — or whether it would work standalone or integrate readings from an external CGM device like Dexcom’s or Abbott’s.
The honest answer is that fully accurate, FDA-cleared non-invasive blood glucose monitoring integrated into a consumer wearable does not yet exist. The technology is under active, well-funded development by some of the world’s most capable research organizations. The convergence of machine learning for signal interpretation, advances in optical physics, and miniaturized wearable hardware is narrowing the gap. But the physiological challenge is real, the regulatory bar is appropriately high, and the history of this field cautions strongly against attaching specific commercial timelines to any particular research program’s progress.